Call it the era of American longevity: Currently, approximately 35 million citizens are 65 or older, a tenfold increase over the past century. Moreover, that population is set to double by 2030, as a flood of baby boomers reaches retirement age. Yet, as lifespans extend, health conditions associated with aging will also reach unprecedented prevalence. The National Council on Aging reports that 77 percent of older adults have two or more chronic diseases, meaning the nation’s health care needs will soon multiply. Mental health disorders are also set to rise sharply: By 2030, 15 million older Americans will face challenges such as depression and dementia.
In this project, we set out to explore various measures of well-being among older individuals, comparing their health indicators with those of other age groups. To do so, we analyzed data from the Centers for Disease Control and Prevention’s (CDC’s) Behavioral Risk Factor Surveillance System, a comprehensive annual survey of more than 400,000 Americans. Our findings reveal the health obstacles older adults are currently confronting and how they typically accumulate across a lifespan. Additionally, we studied preventative measures such as exercise and elders’ experiences seeking medical care. To get the real story of how older adults are struggling and succeeding in their efforts to stay healthy, keep reading.
Decline Over Time
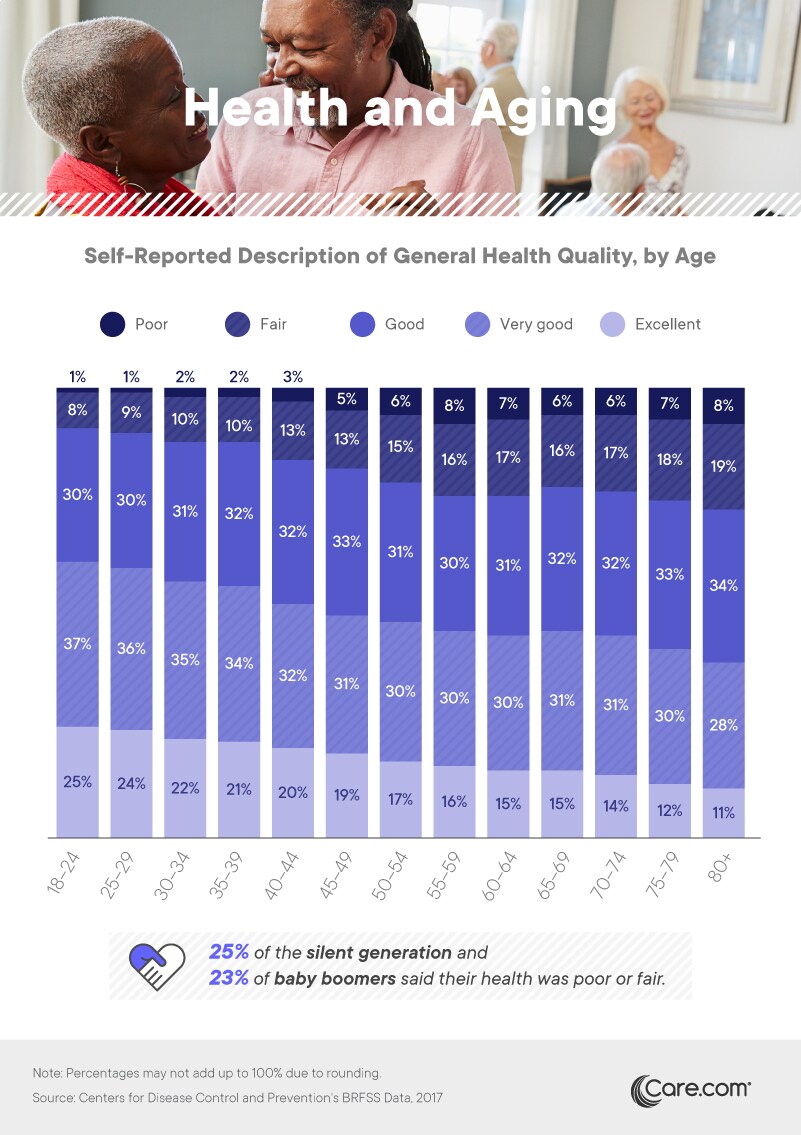
It’s no secret that health problems emerge across the human lifespan, but our data present this trend with compelling precision. Among those aged 18 to 24, just 9 percent said their health was poor or fair. Among individuals 80 and older, just 39 percent said their health was very good or excellent. Indeed, experts note that while chronic illnesses are more common after middle age, the exact age of onset can vary substantially. Type 2 diabetes, for example, is typically diagnosed in patients older than 45, but complex hereditary and behavioral risk factors mean the disease can emerge at practically any age.
In reviewing these results, it’s important to distinguish between the self-reported perceptions of well-being presented here and the medical community’s standards for healthy living. One recent large-scale study conducted by researchers at the University of North Carolina concluded that just 12 percent of American adults qualified as “metabolically healthy.” With regard to older adults, this distinction is cause for particular concern. If 25 percent of the silent generation and 23 percent of baby boomers report their health is fair or poor, how many more might actually belong to these categories?
Physical Hurdles vs. Mental Health
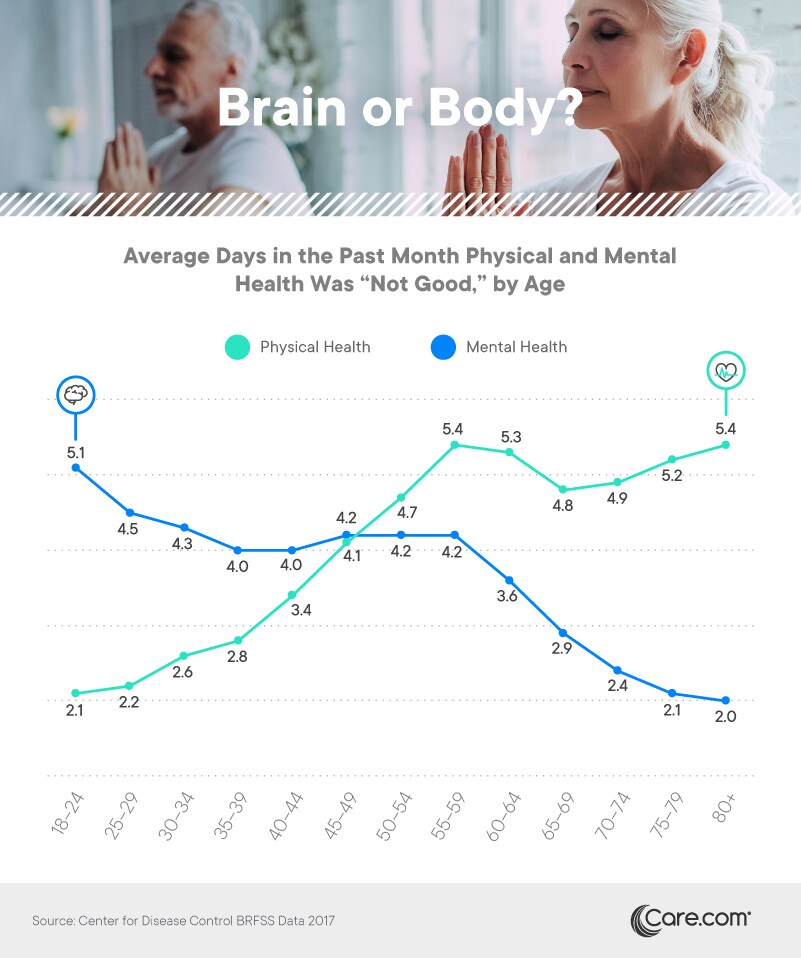
Among younger Americans, psychological and emotional challenges seem to outweigh physical obstacles: Individuals aged 18 to 44 reported considerably more days each month in which their mental health was “not good.” This pattern was most evident for those 18 to 24. While they may be physically robust, college-aged individuals are particularly prone to mental health challenges. By the age of 45 to 49, however, mental and physical health challenges seem equally problematic. On average, individuals in this group reported roughly four difficult days of each kind per month.
Interestingly, mental health challenges appear to decline in each successive age range after 60, even as individuals report serious physical health problems on approximately five days per month. Experts say older persons face an increased risk of conditions such as depression, especially if they suffer from physical ailments as well. But authorities also note that many older adults do not identify their experiences as mental health issues, dismissing their own feelings of sadness or loneliness. Accordingly, they may not report difficult mental health days as often as younger generations despite significant struggles.
Insufficient Exercise?
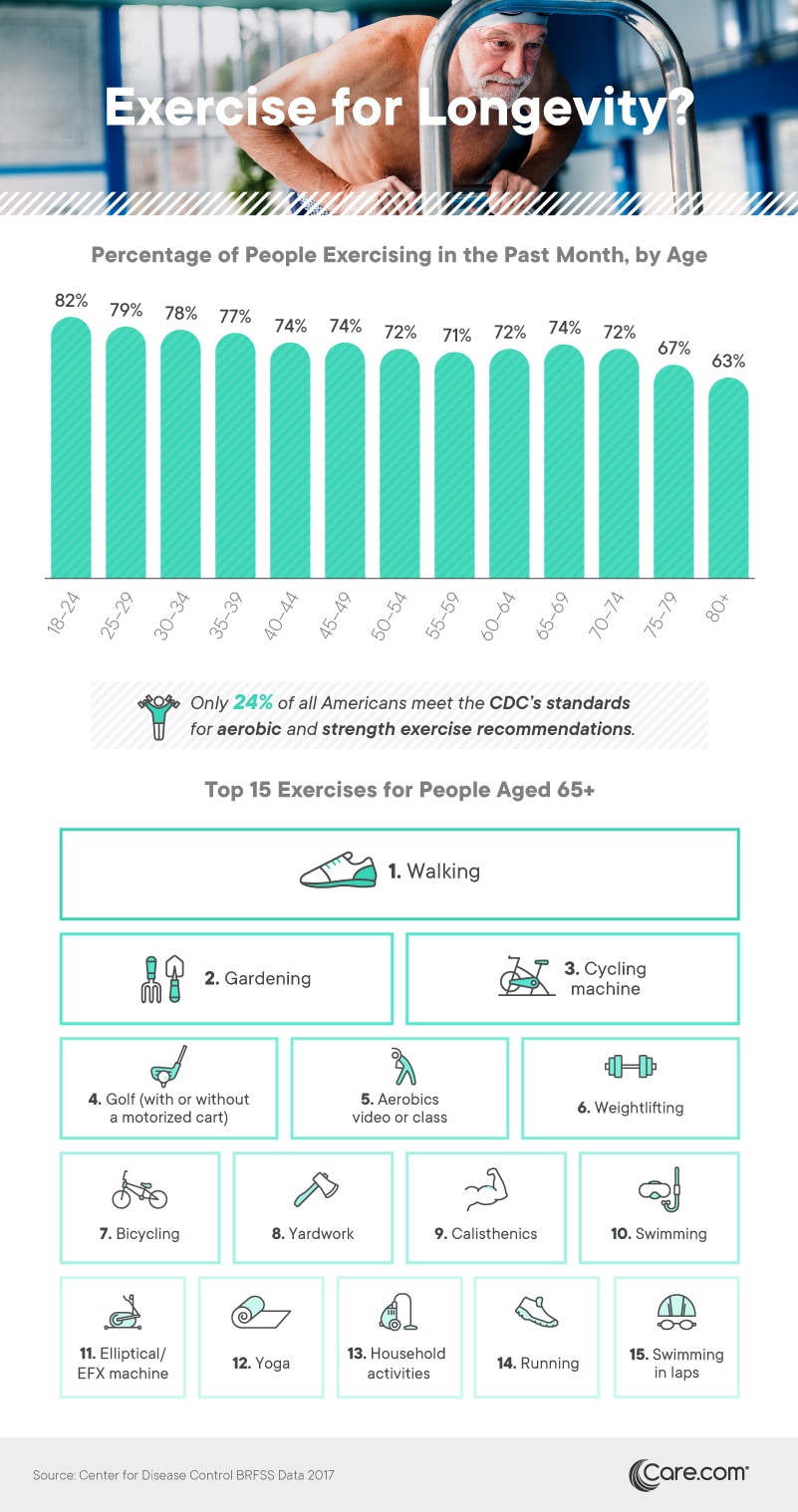
Rates of exercise declined gradually across age groups: While 82 percent of those aged 18 to 24 exercised at least once in the last month, just 63 percent of people 80 and older said the same. Of course, experts recommend a far more active exercise routine than merely once a month, and improvement is necessary across age groups. In fact, our data indicate that less than a quarter of Americans meet the CDC’s physical exercise guidelines. This lack of physical activity has massive consequences for the country, including increased rates of chronic disease and $117 billion in associated medical expenses each year.
Americans 65 and older seemed particularly drawn to certain kinds of exercise, however, including activities that might bring them outdoors, such as walking and gardening. Bicycling was also a common pastime, although older adults used indoor stationary bikes more often than they actually hit the road. Additionally, golf, the classic retirement pursuit, remained a common form of exercise for seniors. However, some doctorsbemoan the sport’s declining popularity, fearing that future generations will miss out on its health benefits.
Geography of Elder Activity

When it comes to older Americans getting active on a regular basis, no region quite compares to the West Coast. California, Washington and Oregon each ranked among the top 10 statesin terms of the percentage of senior residents exercising at least once in the last month. Even further west, Alaska and Hawaii also had strong rates for elder exercise. On the East Coast, at least 75 percent of elders in Vermont, Connecticut and Maine exercised recently. It’s no accident that many of these states boast some of the longest average lifespans in the nation: Even light activity can extend one’s life expectancy.
Conversely, in many Southern states, less than two-thirds of residents aged 65 and older exercised in the past month. To be fair, these trends are not limited to older individuals. Public health officials warn that exercise rates in many Southern states are poor across all age groups. It’s hard to plan consistent activity when you’re miles away from the nearest gym or park. Indeed, research shows that older adults living in rural areas are less likely to be physically active than their counterparts in the suburbs and cities.
Harmful Habit
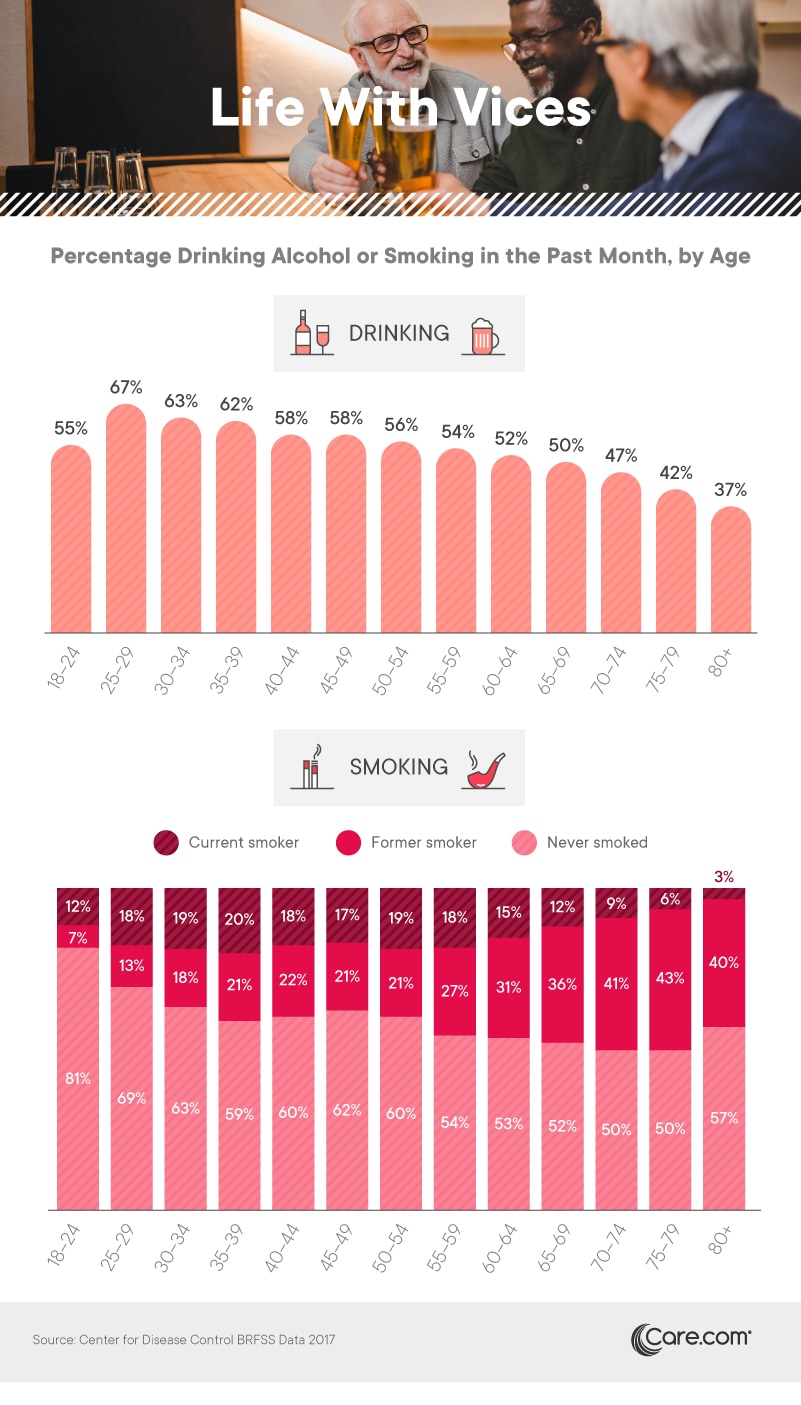
Alcohol consumption was most common among those aged 25 to 29, with roughly two-thirds of that cohort taking at least one drink in the last month. From there, drinking declined slightly in each successive age group. Among those 80 and older, just 37 percent recently consumed alcohol. Yet, experts say older Americans are actually drinking more than in decades past, with a particular rise in alcohol consumption among elderly women. While heavy drinking can prove problematic at any age, indulging excessively can be particularly dangerous for older adults, especially if alcohol interferes with the function of essential medications.
With regard to smoking, individuals aged 18 to 24 were most likely to report never having used cigarettes (perhaps because tobacco use has been eclipsed by vaping among young people). Conversely, at least 40 percent of people aged 70 and older reported smoking in the past. These data are roughly consistent with past smoking trends: Throughout the ’60s and ’70s, more than a third of Americans reported having a cigarette in last week. Thankfully, only a small portion of seniors continues to smoke currently, although mortality remains substantially higher for past smokers than for those who never picked up the habit in the first place.
Medical Schedules
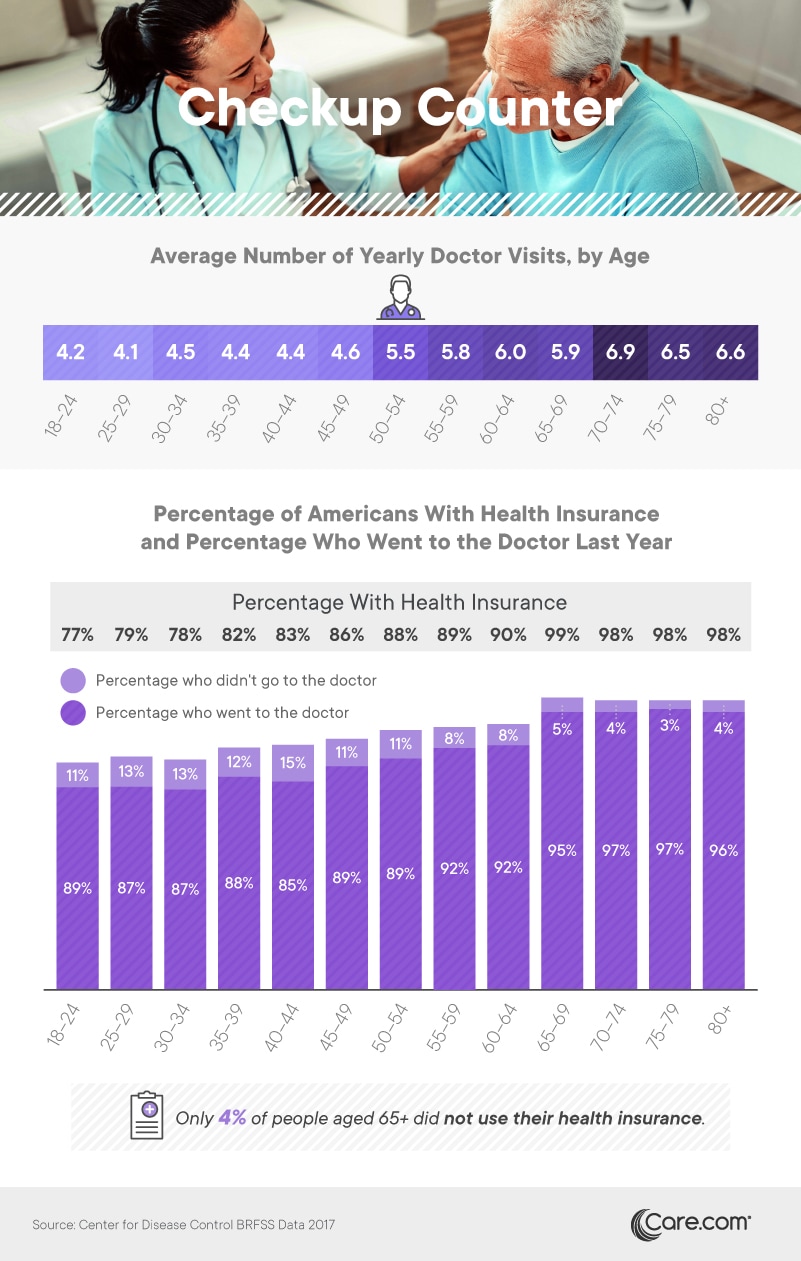
Although young people require less medical care than their elders, the average young American does see the doctor on multiple occasions each year. In fact, those aged 18 to 49 visited the doctor between four and five times on average – all the more reason that insurance is a smart investment even for the young and healthy. Unfortunately, less than 80 percent of adults under 35 had coverage of any kind. Many among this cohort are too old to utilize their parents’ coverage but are unwilling to purchase their own through exchanges established by the Affordable Care Act. In fact, officials say individuals between 18 and 34 represent 40 percent of the potential exchange market, but only a quarter of actual customers.
At the other end of the age spectrum, all but a tiny fraction of seniors said they had have health insurance. This finding reflects the availability of Medicare to all citizens who reach age 65, and the vast majority of older adults seem to make use of their coverage. Ninety-six percent of seniors 80+ with insurance visited the doctor at least once in the last year. Because nearly 60 million people possess Medicare coverage currently, the program is among the federal government’s most expensive services, with payouts totaling $702 billion in 2017.
Insurance as We Age
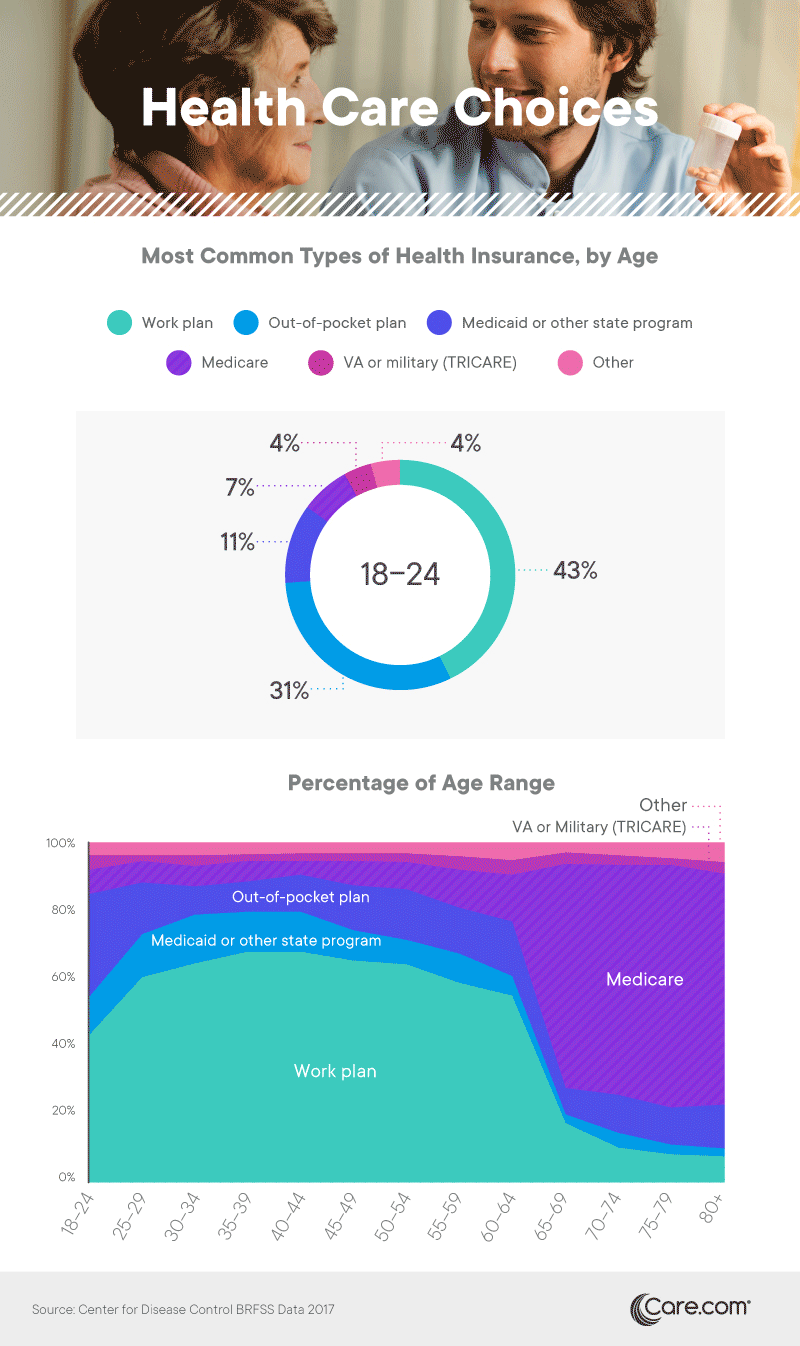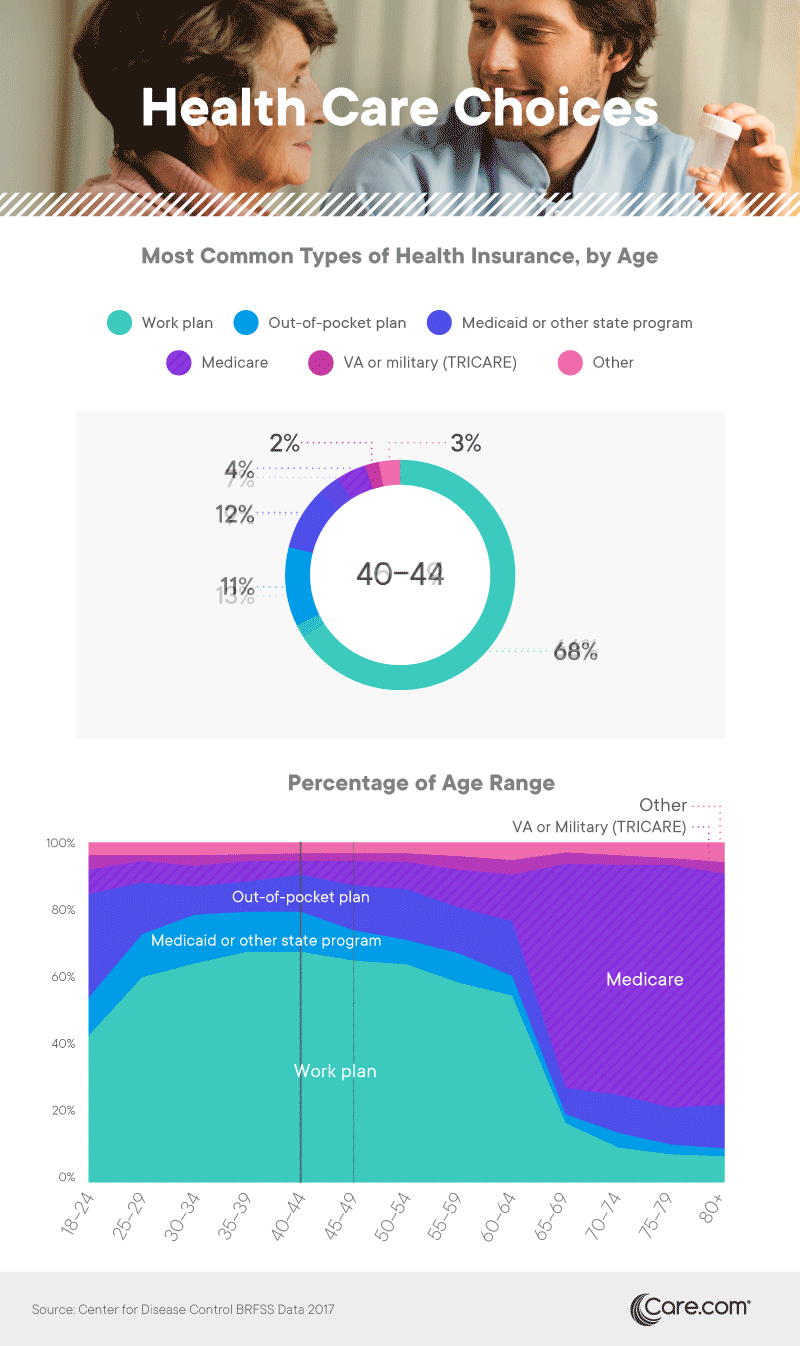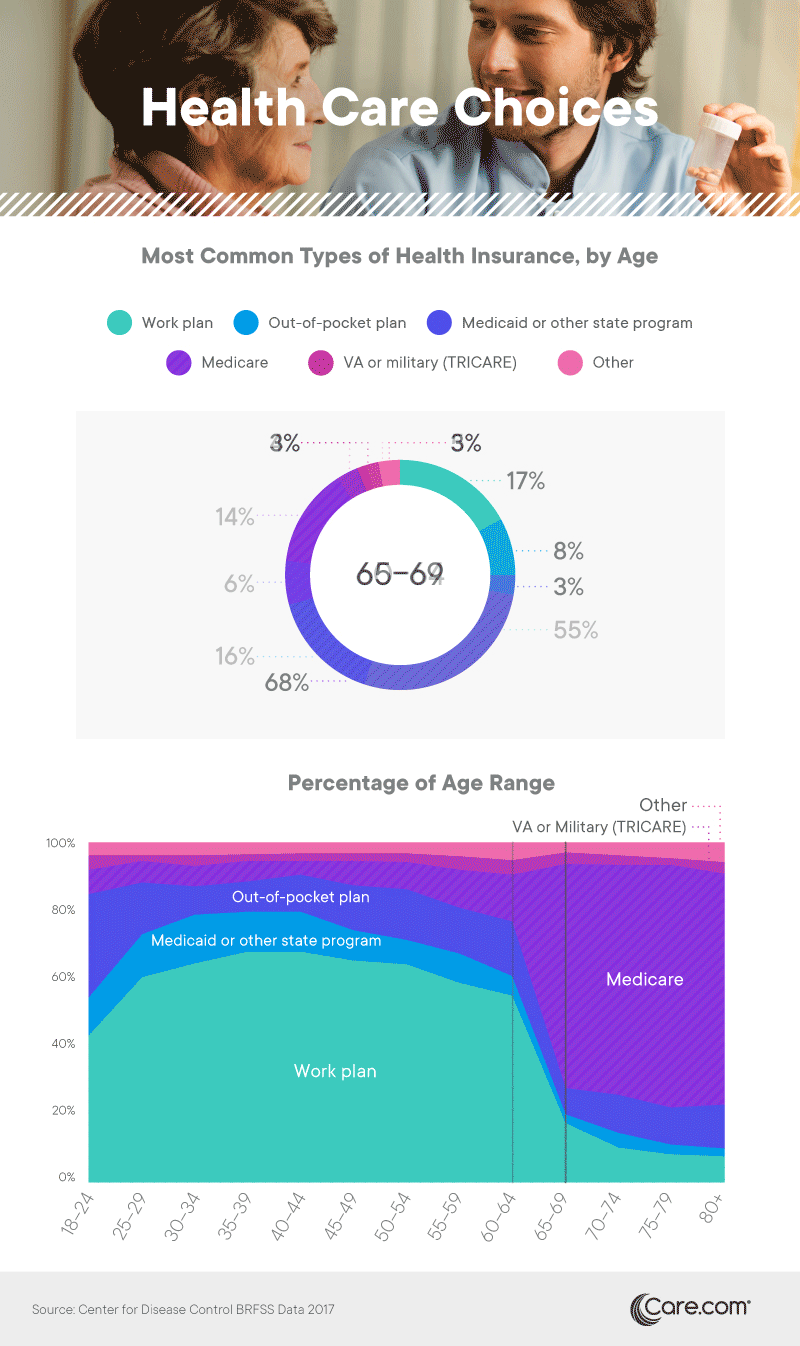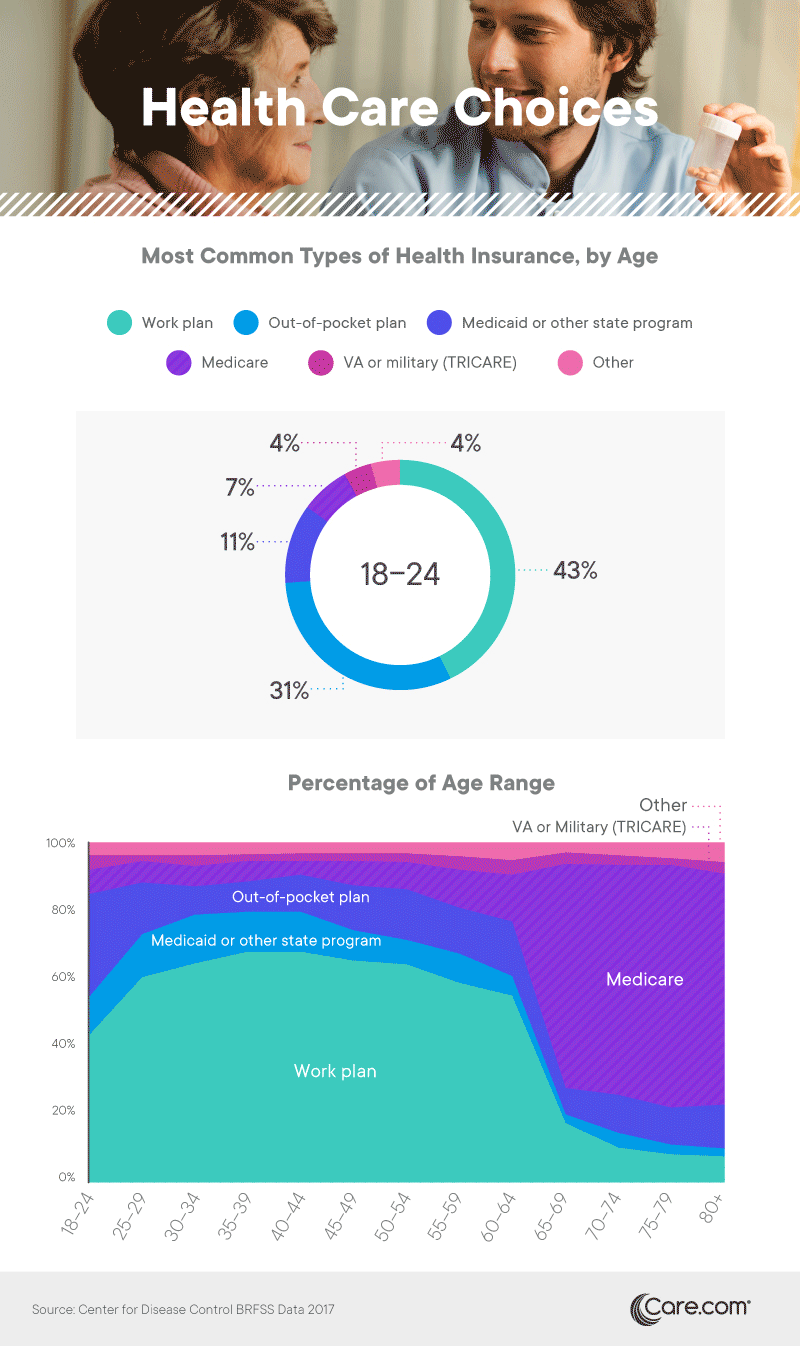
Among Americans younger than 65, those with insurance primarily obtained it through employer-based plans. While the Affordable Care Act created penalties for large companies that failed to offer insurance to their employees, roughly half of small businesses offer health plans as well. Another large segment of Americans younger than 65 paid out of pocket for their plans, obtaining insurance as individuals or as a family unit. Many of them utilized tax credits meant to offset the cost of insurance policies obtained through the marketplace, a significant cost savings for individuals with lower incomes.
While Medicare was the dominant option among seniors, other forms of insurance provided by the government also covered substantial portions of the population. Federal VA benefits covered a small percentage of adults, while Medicaid or other state programs were particularly common for those aged 25 to 44. Of course, federal health care programs also cover a much younger cohort. More than 35 million children have currently enrolled in Medicaid or CHIP coverage.
When Price Prevents Care
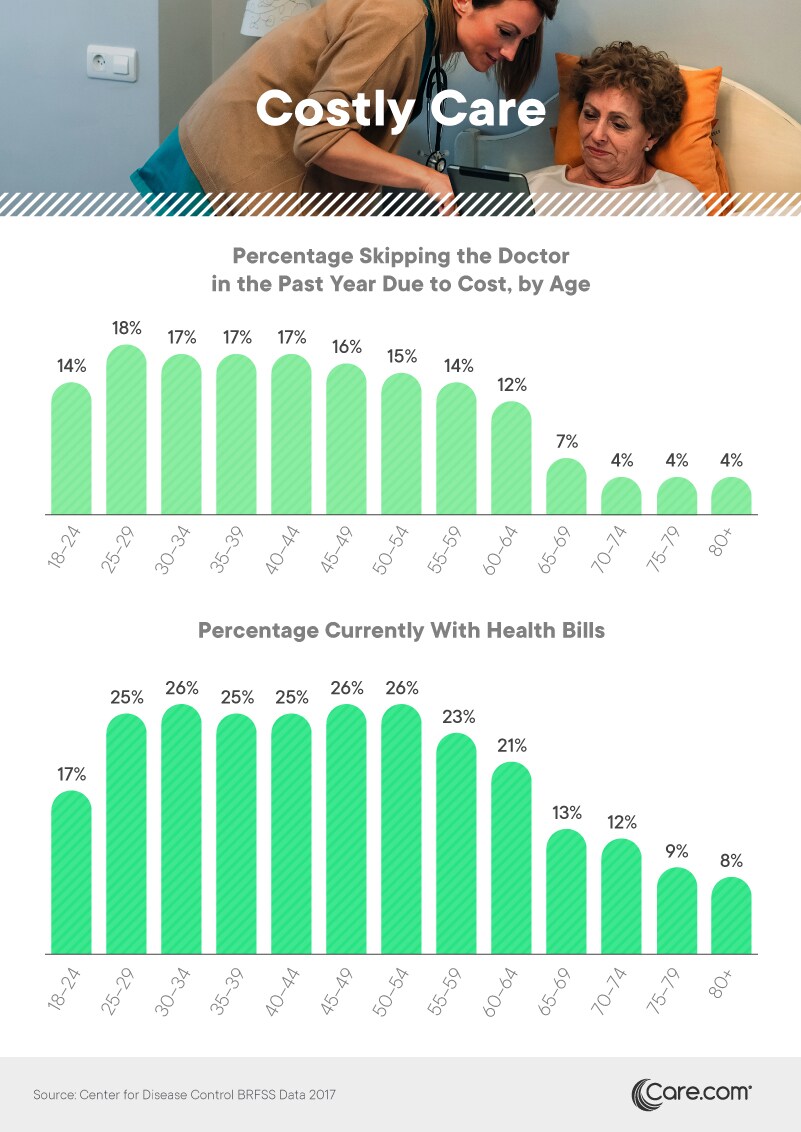
As health care costs continue to rise, the specter of medical debt is increasingly intimidating: One recent study found that Americans are more fearful of large medical bills than an illness itself. Those aged 25 to 29 were most likely to skip a doctor visit for cost reasons – no accident, given this age group had the lowest rates of insurance coverage. But even among middle-aged Americans, skipping care to avoid expense was relatively common. Of course, such a decision could backfire disastrously if a minor problem goes untreated and eventually becomes a medical crisis.
Outstanding health bills were also quite common among young and middle-aged adults. From age 25 to 54, at least a quarter of Americans had health-related financial obligations. Unfortunately, unpaid medical debts are frequently referred to collections agencies, even if the total owed is just a few hundred dollars. Among seniors, unresolved medical bills were relatively uncommon, thanks largely to Medicare coverage. Still, Medicare recipients can still face large bills for certain services, including outpatient care that isn’t entirely covered. As a result, more than 1 in 10 individuals aged 65 to 74 still had outstanding medical bills.
Compassion – and Action
Our findings suggest that significant health concerns are quite common among older Americans, producing challenges related to medical costs and quality of life. And while most older Americans possess insurance coverage, a substantial percentage still struggles to afford health care necessities. Moreover, older adults too often forego preventative measures, such as exercise and abstinence from alcohol. If these conclusions seem troubling currently, these issues will only intensify as the elderly population expands. From national policy to state and local efforts, communities must respond to this rising tide of need throughout the nation.
Of course, Americans must begin by considering care for their own family members. If someone you love requires assistance, excellent care may be more affordable than you imagine. Care.com provides an easy-to-use platform for families to hire senior care providers, with a seamless system for reviewing references and conducting background checks. Whether your loved one needs in-home help or compassionate companionship, you can find the right caregiver on our site. To see how easy it is to get started, explore our site today.
Methodology and Limitations
To compile the data shown above, we looked at the CDC’s Behavioral Risk Factor Surveillance System 2017 survey data for differences in health and health care between older and younger demographics. We decoded over 400,000 rows of data in the combined landline and cell phone data set using information provided on the CDC’s website, and all percentages were computed using the stratum weight assigned to each line entry.
Because the data collected were a survey, it is susceptible to criticisms and biases common to any survey, such as telescoping and recency biases. All efforts were made to provide the data as taken directly from the BRFSS data, and the numbers were rounded to the nearest percentage point.
Sources
- https://abcnews.go.com/Health/story?id=118056&page=1
- https://www.ncoa.org/news/resources-for-reporters/get-the-facts/healthy-aging-facts/
- https://www.cdc.gov/brfss/index.html
- https://www.medicalnewstoday.com/articles/317375.php
- https://www.unc.edu/posts/2018/11/28/only-12-percent-of-american-adults-are-metabolically-healthy-carolina-study-finds/
- https://www.pewresearch.org/topics/generations-and-age/
- https://www.webmd.com/depression/news/20180910/1-in-5-college-students-stressed-consider-suicide#1
- https://www.cdc.gov/aging/mentalhealth/depression.htm
- https://health.gov/paguidelines/second-edition/pdf/Physical_Activity_Guidelines_2nd_edition.pdf
- https://edition.cnn.com/2018/10/24/golf/golf-health-report-spt-intl/index.html
- https://www.businessinsider.com/ranked-life-expectancy-by-state-2018-4
- https://time.com/5166564/physical-exercise-can-increase-lifespan/
- https://www.inc.com/jeff-haden/the-cdc-just-ranked-every-us-state-by-how-much-people-exercise-and-things-aint-pretty-down-south.html
- https://www.americashealthrankings.org/explore/senior/measure/physical_inactivity_sr/state/ALL
- https://www.cnn.com/2017/03/31/health/older-adults-drinking-study/index.html
- https://www.cnn.com/2018/04/06/health/high-schools-vaping-epidemic/index.html
- https://www.cdc.gov/tobacco/data_statistics/fact_sheets/health_effects/tobacco_related_mortality/index.htm
- https://time.com/5052313/health-insurance-obamacare-challenges/
- https://www.hhs.gov/answers/medicare-and-medicaid/who-is-elibible-for-medicare/index.html
- https://www.kff.org/medicare/issue-brief/the-facts-on-medicare-spending-and-financing/
- https://www.kff.org/infographic/employer-responsibility-under-the-affordable-care-act/
- https://www.inc.com/associated-press/health-benefits-vanish-small-business-only-half-offer-today-2017.html
- https://www.va.gov/health-care/about-va-health-benefits/
- https://www.kff.org/medicaid/state-indicator/total-medicaid-and-chip-child-enrollment/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D
- https://www.cnbc.com/2018/04/22/why-health-care-costs-are-making-consumers-more-afraid-of-medical-bills-than-an-actual-illness.html
- https://www.cbsnews.com/news/even-small-medical-debt-can-be-big-trouble/
- https://www.forbes.com/sites/forbesfinancecouncil/2018/05/24/how-to-avoid-medical-debt-in-your-retirement/#38fe0c8b6d66
Fair Use Statement
Too often, the challenges facing older Americans go ignored in our public discourse. Accordingly, we hope you’ll share this content with your friends and loved ones so that they can join the conversation about caring for our elders in the years to come. If you do share our work, link back to this page so that others can discover the full story. Please use this project’s graphics and information for noncommercial purposes only.

